Anti-Fibrotic Activity of Protein SCGB3A2 in Mice Could Lead To New PF Therapies
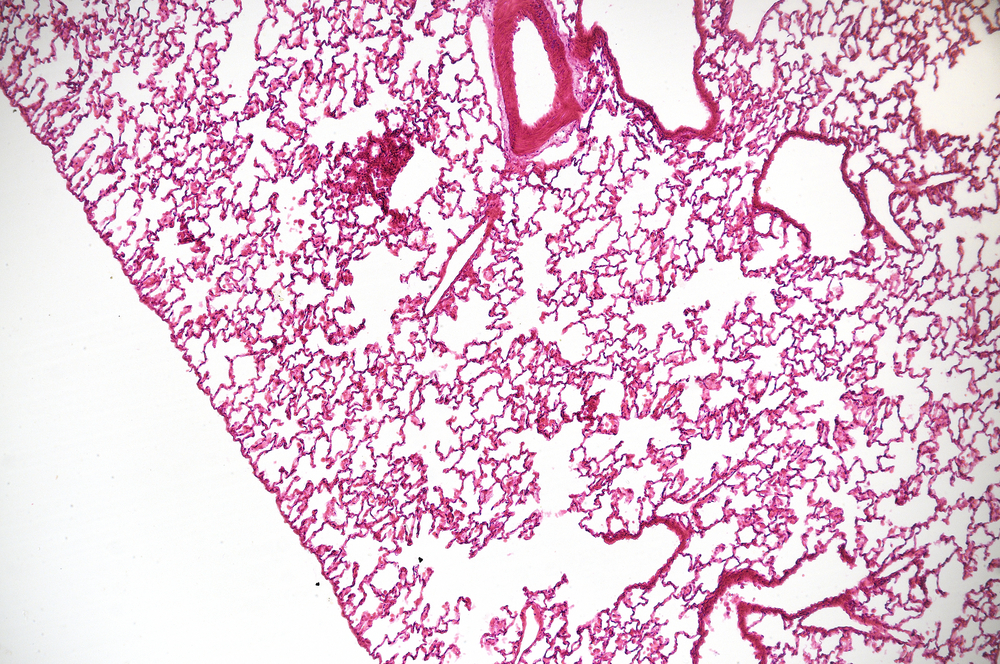
A protein expressed solely by cells lining the airways is at the center of an interesting new strategy that may help fight pulmonary fibrosis. The protein, secretoglobin (SCGB) 3A2, was investigated during a recent study conducted by the Laboratory of Metabolism at the National Cancer Institutes in the National Institutes of Health. The research team confirmed that SCGB3A2 has anti-fibrotic activity and prevents mice from developing severe pulmonary fibrosis.
Until this study, researchers had not investigated SCGB3A2 inside an animal model relevant to pulmonary fibrosis. “While SCGB3A2 is known to have anti-inflammatory, growth factor, and anti-fibrotic activities, whether SCGB3A2 has any other roles, particularly in lung homeostasis and disease has not been demonstrated in vivo,” explained the authors of the study, “Transgenically-expressed Secretoglobin 3A2 Accelerates Resolution of Bleomycin-induced Pulmonary Fibrosis in Mice,” which was published in BMC Pulmonary Medicine.
The mice used in the study were genetically designed to express extra SCB32A in the lungs. This caused their lung cells to express five-times more SCB32A than is normally produced. Expression was found exclusively in alveolar type II cells and airway epithelial cells, indicating that the researchers were able to control what areas were affected by the SCB32A transgene. Additionally, the mice grew to demonstrate normal lung function.
To test the ability of the mice to resist pulmonary fibrosis, the researchers attempted to induce the disease in the mice using bleomycin, a commonly used agent for triggering pulmonary fibrosis. While the SCGB3A2 over-expressing mice initially showed a large amount of fibrosis three weeks after injury, they quickly resolved their pulmonary fibrosis six weeks after injury. The rate of resolution was significantly different than that of mice without an SCGB3A2 transgene.
“The decrease of fibrosis coincided with the increased expression of SCGB3A2 in Scgb3a2-transgenic lungs,” wrote the authors. With good overlap of SCGB3A2 and areas of low fibrotic activity, the authors believe a therapy that uses SCGB3A2 gene delivery may be a feasible new option of treatment of pulmonary fibrosis.






