My Memories of Transplant Recovery: Hallucination and Defibrillator Paddles
Written by |

When I write about my lung transplant, I honor my donor, for whom I am forever grateful.
I didn’t know him, but I know he was a caring person. Last August, I was the lucky recipient of his lungs, which changed my life like nothing else has, or ever will.
When I think about the day after transplant and how my recovery went, a few things come to mind:
- My hallucination
- A pair of defibrillator paddles
- The new nickname “Double Derriere”
- Restricted visiting hours
My surgeon said recovery takes a year. Additionally, he said I would have several up days and down days. Thus, I must have self-restraint in my recovery.
I had my share of rising and falling days emotionally. Remember, each transplant recipient experiences their own unique recovery, and my case is no different.
My first day was a low point. Click, click, click on the roller coaster.
Hallucination
On Aug. 14, 2020, at 9:30 p.m., a surgeon completed my lung transplant. Hospital staff brought me out of an induced coma the next morning and took me off the ventilator.
While waking up, I hallucinated, believing I was coming out of anesthesia. I felt like I could barely open my eyes. Next, I sensed that two nurses were about to take out my endotracheal tube, but that didn’t happen. And the next thing I envisioned was a janitor wearing a brown coat pushing a cart down the hallway.
After the janitor scene, I returned to picturing the two nurses trying to take out the breathing tube. It felt like I was in the movie “Groundhog Day.” I imaged opening my eyes a little more, thinking the tube would come out now. But my hallucination skipped to the janitor in the hallway.
Once again, I returned to the beginning of the delusion. I tried moving my fingers and opening my eyes more, and visualizing my hands. But something blue that looked like boxing gloves had been wrapped around both of my hands. That turned out to be hospital staff wrapping my hands with gauze and blue tape to keep me from pulling on the tubes.
This hallucination continued until I finally was off the ventilator.
I asked the doctor and nurses how many other patients usually experience hallucinations. They said it happens occasionally, but that it’s rare.
Defibrillator paddles
Later in the day, my 5-foot-2-inch nurse wanted me to move from the bed to a chair. I sat up in the bed. She told me to take my time at the edge of the bed.
As a graduate of the U.S. Military Academy at West Point, I was trained not to fail any challenges, no matter what. We were taught to do whatever it takes to succeed. So, after waiting a minute or so, I used my West Point training to move to the chair.
But when I stood up, my head started spinning. The nurse asked if I was OK. She said I should focus and breathe.
The next thing I knew, I was in the chair with one derriere on and one derriere off. I had passed out for about 20 seconds. The room was full of people, and one nurse even brought defibrillator paddles. Seeing all of those nurses — especially the one with the paddles — horrified me. I didn’t know who was more upset, the nurse or me.
In hindsight, I suspect that I had torn two small holes in the clamshell incision on my left side. These two small holes eventually caused issues with my recovery. This incident showed me that I needed to take things slowly and carefully. It was all about building more of my West Point character.
I told my friends about the incident, how the petite nurse had guided me into the chair, and how I had one derriere on and one derriere off the chair. In response, my West Point friends nicknamed me “Double Derriere.” So, I am on the Double Derriere Vertical Loop forever.
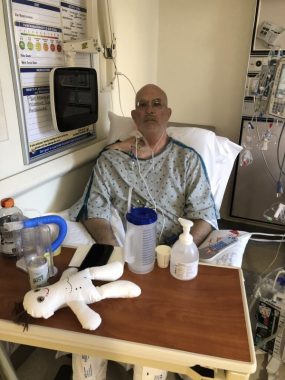
After struggling, columnist Kevin Olson sits in a chair at the hospital following transplant, on Aug. 18, 2020. (Photo by Dana Olson)
Visiting hours
My day didn’t improve too much after the first two incidents. I was allowed to have a visitor from noon to 8 p.m. Before that, I needed to get the results of my post-surgery COVID-19 test, but a new COVID-19 policy at the hospital delayed the results.
After passing out, I was distraught, and I needed to see a family member. After the operation, I had only spoken with my wife, Dana, and my daughter, Terri.
Finally, around 6 p.m., I was allowed to see someone, so I asked for Dana. The COVID-19 restriction allowed me to see only one person a day. It was hard for me not to see Terri, and I know she was upset about it. We talked before the surgery, but we hadn’t been able to see each other, which was emotionally challenging.
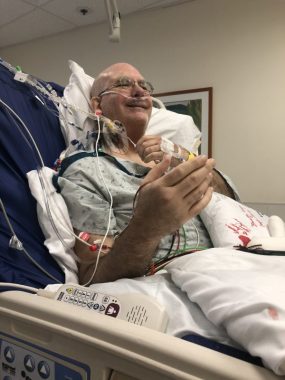
Kevin smiles at his wife, Dana, following his transplant surgery, on Aug. 15, 2020. (Photo by Dana Olson)
Have you or a loved one faced recovery following transplant surgery? How was your experience? Please share in the comments below.
***
Note: Pulmonary Fibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Fibrosis News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to pulmonary fibrosis.




Karen Pratt
I had a transplant in Oct of 2020..it went much smoother than you described, however, I did have hallucinations, of the walls breathing and my dogs being in the room with me...I also had delusions, which I told no one about, for fear they would think I had gone off the deep in. I had a reoccurring delusion, that my house keeper's brother was trying to kill me because I had insisted that she wear a mask at my house. He sent killers to my room, killed a pregnant nurse, tried to kill me several times, then when he would not succeed, he sent my house keeper to kill me, who apologized deeply for having to kill me...oh well I am still here and doing great, inspire of the delusions. I think it was related to medications ......
Kathryn Bottaro
My fiancé had one more test before going on transplant list. We were so hopeful On Saturday he passed of cardiac arrest. His oxygen got so low there was no saving him. I feel guilty I didn’t take him in ambulance sooner. I can’t live without him. I wish we made it because I know how much he wanted to live again
Kevin Olson
Kathryn. Sorry for your loss. Praying for you.
Kevin Olson
Karen, thank you for your comment. Hope you are doing well now.
Barry Boyle
Hi Kevin, I am a fellow lung transplant recipient. I received a single lung transplant Oct. 2014. I also had hallucinations immediately after surgery. Very strong drugs are administered for pain relief and to keep you sedated. I would stare at the floor or at the ceilng and mythical half human figures would appear. They would slowly revolve and glide across my field of vision. But I could never see their faces. I was so afraid their faces would be something very evil.These hallucinations lasted a couple of days. I didn't tell anybody about them because I thought I might be going crazy. Someone on the transplant team must have found my behavior very interesting because they asked me to participate in an interview with with a panel of doctors. They kept asking me questions and I must have talked for an hour. I was never told about ther observations or conclusions. I had a complicated recovery but have survived so far. Because my disease was completely unexpected (IPF) my family and I were unprepared for a forced retirement. I had severe depression for more than two years. Thankfully I had strong support from my family because psychiatric counseling is very hard to obtain here in Canada. Thank you putting your story out there. I can definitely relate to it. Post transplant I have a vry different life now but I'm still glad to be alive.
Kevin Olson
Barry, Thank you for sharing your story. I had only one hallucination post-transplant. When I was four years old, I had one while I was under anesthesia. Those are the only times I had them. Yes, it would have been interesting to read the results of your interview. Happy to hear you are doing well and you inspire all of the new transplant recipients.
Sharon Goble
I have IPF and find this very interesting!
Kevin Olson
Thank You for reading my story.