Surviving My Pulmonary Function Test
Written by |

I recently completed a pulmonary function test at my local hospital. This test was ordered by my doctor to measure how well my lungs take in and exhale air, and how efficiently my lungs transfer oxygen into my bloodstream.
It is a noninvasive test, and I did it as an outpatient. I have this test done every six months.
Mixed feelings
I always have mixed feelings about doing this test. I’m grateful for it, because it gives me real numbers to assess my lung health and the progression of my disease. I also feel nervous about this test, because it is so exhausting. Here’s what I’ve learned and experienced when going through a pulmonary function test.
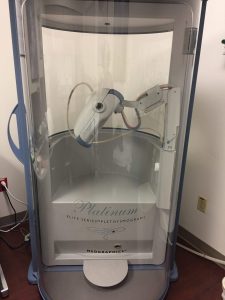
I took a few pictures while I was there to show you what it’s like. You sit in a clear, sealed box that controls how much oxygen you breathe when not using supplemental oxygen.
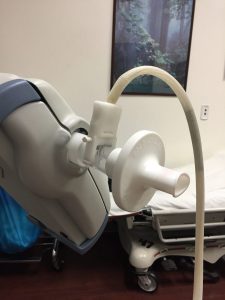
You breathe in and out of a mouthpiece in very specific ways, such as slowly or fast as possible. These breathing tests are done in sets of three to make sure an accurate finding is determined.
Diffusion capacity (DLCO), is another measurement during the pulmonary function test. This is measured when the patient breathes carbon monoxide for a very short time, often one breath. The difference in the amount of carbon monoxide inhaled, and the amount exhaled, gives an estimate of how quickly gas travels from the lungs to the bloodstream. This is important because the amount of oxygen in our bloodstream is a huge part of what keeps our organs and system going.
Much needed information
As you can see, having a pulmonary function test gives pulmonary fibrosis patients much-needed information. The test usually takes about an hour or more, and it’s extremely tiring for me to go through. The time to perform this test has gotten longer as my PF has progressed, because I need to rest longer and use supplemental oxygen between the tests. Several of the tests require you to breathe in as much air as possible, as quickly as possible. This makes me cough terribly, and it takes a while with little sips of water to recuperate.
I used to be able to drive to and from the test myself, but I’m no longer able to do that. I’m still able to drive to the appointment, but can’t drive home, because I’m too exhausted. I’m grateful to my husband for coming with me.
This test is hard to go through, but it’s worth the effort. It provides my doctors and me with the information we need to assess my lung health and the progression of my disease. I always ask for a copy of the preliminary test results before I leave, because I like to compare my current results with prior results.
How about you?
I hope this information is helpful to you. I’d love to hear about your experience taking a pulmonary function test. You can get more information by visiting the Johns Hopkins website.
Has your doctor made a referral for you to have a pulmonary function test? What was it like for you? How does it help you and your treatment?
Please leave a comment below, and share with those who could benefit via email or on social media. We’re in this together!
***
Note: Pulmonary Fibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Fibrosis News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary fibrosis.






Carol
I'm glad to know that you were exhausted after test, so was I and was concerned. It does take a lot out of you.
Kim Fredrickson
Thanks Carol...it is concerning, but is very normal. I'm glad they are only every six months!
Deisy Haney
I thought I was being wimpy. Was glad to see this article. I feel drained. This was my first PFT. I am praying for not to serious report.
Larry
Hi! Kim, And MERRY CHRISTMAS, I' going for my PulTest on Thurday 2St. An like you I'm going with some apprehension. I have diabetes and a unknown ticker problem and feel(in my mind) that all my problems are related to the IPF. My Cardo and other functions are normal ,except for the blood sugar levels being hard to control since I'm not being to active. I t must be remembered that each of us who are tagged with this disease (IPF) have different sub issues which effect our well being. With that you did a great job of explaining the Lung function test, and where to go to get more information, that's great, keep it up . Thanks Larry
Kim Fredrickson
Hi Larry, Thanks for your comment. Hope you had a wonderful Christmas. I hope your PFT goes well. So sorry you have to deal with diabetes and cardio issues too. You're right it is common to deal with additional issues besides PF. Thanks for your encouragement about my column. It means a lot to me.
Bob Bradley
I take a PFT every three months and it is exhausting. My question is this, how accurate are the results? Since I was diagnosed with IPF a little over a years ago, my test results have fluctuated very little. While that's good news, I do feel like I am getting worse, having more difficulty breathing & using more supplemental oxygen. Are these tests truly accurate?
Kim Fredrickson
Hi Bob...every three months? That does sound exhausting! Great question wondering how accurate they are. My personal experience is that they are very accurate for me: meaning the results reflect how I'm feeling and changes in O2 use. How frustrating that is different for you. Darn! I wish I could offer an idea as to why that is.
Maribel Gonzalez
I feel the same too. I jokingly call it the torture chamber. I had noticed though that some technicians are very understanding and helpful which makes it easier and relieves some of the stress. I had dealt with technicians that are less sympathetic and certainly that is not helpful.
Kim Fredrickson
Hi Maribel...I totally agree. I go to a hospital a little farther than I have to, in order to get the same kind technician each time. It makes such a difference! Many blessings to you.
JOHN SLIWINSKI
I feel the first test is usually a baseline for the doctor. After that the results are compared to the first one which gives them an idea of your status. I get them every six months I like to see where I stand compared to the first time I took the test. I like to have positive results. Let your md interpret the results and their accuracy and give you the scope of how you are doing. Without these tests how would you know where you stand with IPF.
Kim Fredrickson
Hi John, thanks so much for sharing your wisdom. I completely agree! It really is an objective way to monitor how our disease progresses. Thanks for your comment.
Kevin Krambeer
PFT is a useful tool although any one specific test results can vary, perhaps as much as 10%, so better to look at trends over time. Just as important are your HRCT, 6 minute walk, listening to lungs and how you feel according to my transplant team. Wish all this was easier too.
Kim Fredrickson
Hi Kevin, so very true...there are many measures to get an accurate assessment of our lung functioning.
Joyce Douglas
Hi Kim. I was just diagnosed in May of 2017 with IPF. I had to do a Breathing Test, or Lung Function Test while in the hospital to help with the diagnosis to make sure that was what I really did have. I did find it tiring for sure. But, haven't had one since...(now nearly the end of Dec.). My Dr. said that the blood oxygen test (needle into artery to measure with and without the oxygen) was sufficient. I hope so. Not sure what else to expect. Thank you for the msg. I will be sure to rest up for the test. Don't enjoy the walking 6min. test either as I was very tired after the first one. Then the Respirologist set the oxygen up at 4l and that was an improvement. Merry Christmas.
Kim Fredrickson
Hi Joyce, Thanks so much for sharing. I know it is so much to adjust to after recently being diagnosed. I hope you had a Merry Christmas too :)
Kathy Fowler
Well you described it exactly as I would have. The only relief I seem to get is after my test I get a breathing treatment. That helps so much more than just a few hits off of an inhaler. Thanks for sharing.
Merry Christmas!!
Mary Hilton
What sort of Breathing treatment?
Kim Fredrickson
Hi Kathy, so glad my description matched your experience. I don't get much help from the breathing treatment. So glad it is a help to you. Many blessings...
Sandra
HI Kim it is always a pleasure hearing from you. I was diagnosed with Lung Fibrosis in 2002, was on Prednisone and oxygen for a few years.For 5 years my lungs for hold there own so I was off the medication and the oxygen. Last year I was put back on the medication for sometime else and then my oxygen level started to dropped so here I am back on the oxygen. Recently I realize that my level was dropping in the 88 sometime....I did the 6 minutes walk numbers were up and down...using 6 instead of 4 now going for a scan of the lungs next month to see what is going on. Taking one day at a time
Kim Fredrickson
Hi Sandra, Thanks so much for sharing your experience. I'm so glad you were stable for so long, but so sorry that you've had to go back on meds and oxygen. I know they are good for you, but it can be discouraging. I'm taking one day at a time too :)
Jon skaggs
Be glad you have the benefit of the chamber, the hospital is small and their equipment isn’t update.
My PFT is done with a person having you to breath in and out of a hose as nightly as you can.
Kim Fredrickson
Hi Jon...oh my, that does sound very hard. Your experience does help me appreciate the benefits of the chamber. I hope your hospital's equipment will be updated for you to benefit. Thanks for sharing.
Frances Moore
Hello. I have the pulmonary function test about once a year. It is not too bad for me because the respiratory therapist is a friend and very kind, I am a retired pulmonary nurse so I worked with her. My last test showed very little change ! I use oxygen at night and sometimes in the day. I take allergy shots once a week. That seems to help !
Kim Fredrickson
Hi Frances, thanks for sharing. You certainly have a lot of experience in this area. So glad your friend is able to administer the test...that really does help. Good to hear from you :)
Lisa D Neal
I have my testing this Friday (Jan 19). I was diagnosed in Jan 2017 and this will be my first testing when I was not having a lung infection. Perfect description of what it is like! My son (who is in denial) is taking me and will be with me during the tests.
Kim Fredrickson
Hi Lisa! I hope it goes well...hopefully much better than when you did it with a lung infection. Best Wishes!
Wendy
I am having that breathing test done this month I am scared to get it done I was told by others in can cause you to not be able to breathe and this terrifies me.Is this true?
Tammy Haney
What is this test for I'm scared to death I worry alot these Dr scares me with all these testes. Please someone tell me something I go on the 30th of July. Is this to get me on th rite meds inhalers or what I'm already on two of them but don't open me up. The test I took awhile back they had me to breathe I. This tube an I give all I could an I got this on my phone about appointment an I'm so so scared the inhalers they give me to use it open me up an I was coughing but felt better. Could this be that they trying to c what kind of medicine inhalers to do or what I read in to this an its scares me. Please someone tell me something please I have 2 kids an grandbabys an i want to be here for them. An this scares me.
Beverly
I just had a pulmonary function test on 8-7-19 I was tired n with sarcoidosis and asthma I felt it was needed but exhausting after I went home that evening I got headaches and right side pains n now it’s 8-9-19 n still have headaches and right side pain n it has seem like my breathing tighter since test is this normal?
Angela Waterford
I've heard that my sister was ordered by her doctor to undergo a pulmonary function test. Maybe she should do this test at a good clinical service that offers this. Thanks for adding that this will give her doctor the much-needed information that they need to know, so I'll help her find a clinic next week.
Lynne
I ended up with a loose cough after my PFTs. Is this normal?