Measuring My Improvement in the Year After Transplant
Written by |

I received my new lungs a year ago, on Aug. 14, 2020. Now it’s time for me to reflect on my quality of life.
Initially, I evaluated my progress by how long I stayed in the hospital. Unfortunately, I failed my goal to leave the hospital at the two-week mark because of health issues. This failure caused depression and concern. Then I learned to use my recovery issues, physical condition, and test results to monitor my progression.
First 45 days: The worst days
In the initial 45 days of my recovery, I saw minimal improvement in my breathing and physical condition. The slow progress kept me distressed. My health issues affected my physical condition and test results, so, I used them as my primary measurement.
I had three main wellness concerns. Firstly, I fainted on the first day of recovery, which led to two small tears in my incision. This haunted me. Because of the openings, I continued to have fluid around my lungs, and it kept them partially collapsed.
Also, the tears leaked a lot of liquid. I felt like Carrie in that movie based on Stephen King’s book of the same name. My hospital gown would be soaking wet, along with my chest and lower body.
Then, around Aug. 25, another complication arose. I thought I had a heart attack, which turned out to be atrial fibrillation. A few days later, I had a transesophageal echocardiogram with cardioversion to get my heart back into normal rhythm.
Another problem was that I had an additional surgery. My surgeon wanted to rough up my chest wall to help the lungs adhere better and to eliminate fluid and air. This procedure is called pleurodesis. Also, he talked about exploring the wound. These two surgeries were combined.
Having another surgery didn’t thrill me. On Sept. 3, I had the surgery, which eliminated all of my previous improvements and caused more pain and dizziness. The surgery also caused me to faint three times, and these falls contributed to my worst day of depression.
To check my physical recovery, I charted my speed on the treadmill. From Monday to Friday each week, I walked on the treadmill for 30 minutes. The following graph confirms how little progress I made.
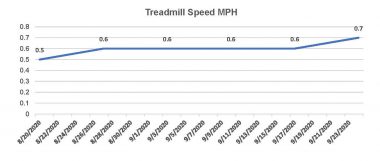
After transplant, Kevin tracked his recovery by tallying his treadmill speed. In the first 45 days, he didn’t see much progress. (Courtesy of Kevin Olson)
Exercise helped, but the overriding factors were my persistent health problems.
The next 135 days: Transition
On Sept. 28, I had a significant recovery breakthrough. A healthcare provider drained 800 cubic centimeters of fluid from around my left lung. It allowed me to breathe easier and eased my pain, which led to a transition from no improvement to speedy progress. Now I could measure my physical condition and lung function and get a meaningful picture.
With my health problems solved, I increased my treadmill speed exponentially, and my lung functions rapidly improved.
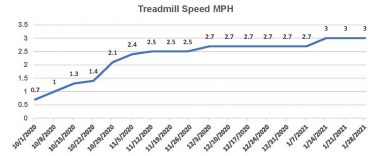
After draining fluid from around his lung, Kevin was able to improve his treadmill speeds in the second phase of post-transplant recovery. (Courtesy of Kevin Olson)
After the transplant, pulmonologists monitored my spirometry forced expiratory volume in one second (FEV1) to detect improvement, as seen below.
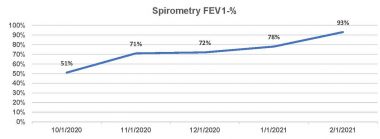
Kevin’s forced expiratory volume in one second chart is more proof of progress. (Courtesy of Kevin Olson)
Now, my worries about recovery were gone. In addition to the empirical data, I noticed a physical and emotional boost.
I had my best day on Oct. 9, when my wife and I went to a park for a walk and to enjoy the scenery. With lots of energy, I walked across a field. However, I had to be careful because of the holes and sticks.

On his best day post-transplant, Kevin went to a park and walked across this field on Oct. 9, 2020. (Courtesy of Kevin Olson)
Next, I had an emotional breakthrough when friends came to visit us, which bolstered my morale. During the visit, my U.S. Military Academy classmates said I needed to pay attention to detail and move my arms 9 inches to the front and 6 inches to the rear. This minor suggestion allowed me to regain my natural balance.
Last 6 months: Fantastic months
In the final six months, my FEV1 continued to rise and stay in the normal range of 80% and higher, as shown in the following graph.
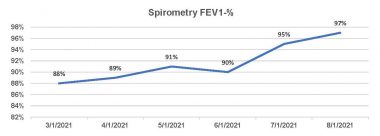
In the last six months of recovery, Kevin’s FEV1 results continued to rise and remain in the normal range of 80% and higher. (Courtesy of Kevin Olson)
At my six-month checkup on Feb. 3, my bronchoscopy showed no rejection or infection.
I finally realized that idiopathic pulmonary fibrosis (IPF) didn’t define me anymore. So, with the IPF barriers lifted, I started challenging myself.
- At the end of February, my wife, Dana, and I drove from Kansas City to Phoenix. My lungs were tested at 7,500 feet, and they passed with flying colors.
- I used stairs whenever possible, which led me to complete the American Lung Association’s Fight for Air Climb.
At my one-year checkup, I did a Snoopy dance. I still had no rejection, which means fewer appointments and labs in the future.
As I’ve shown, my quality of life has improved because of my donor’s lungs. Therefore, I consider Aug. 14 as a celebration of life for my donor. I am indebted to him for his unselfishness.
I am amazed at how much my quality of life has improved in a year. I am looking forward to more challenges, such as flying, in the second year.
***
Note: Pulmonary Fibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Fibrosis News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to pulmonary fibrosis.





Ronald Cole
Kevin thank you for sharing your journey. It was inspiring. Are you still taking anti rejection medication? I read in a study from University of Pittsburgh medical center they are looking at people who ween off the medication.
Kevin Olson
Thank You, Ronald, for reading my story. I am taking low amounts of anti-rejection meds, Cellcept 250 mg twice a day. Prednisone 7.5 mg once a day, and Tacrolimus 1 mg twice a day. My transplant Pulmonologist has not discussed weaning me off the anti-rejection meds. Since I am in my second year, I get labs done every two months. I suspect my pulmonologist won't talk about weaning off the anti-rejection meds until my third year after transplant.
Louise Stotesbury
What a wonderful story. Inspirational and brought tears to my eyes. Not sure I’ll qualify for a transplant here in the UK but so delighted for you. Long may you continue to improve and be well
Kevin Olson
Lousie, happy to hear from you in the UK, and you were inspired. Keep up the faith. Thank you for the wonderful words. Kevin
Jeff Taylor-Jackson
Hi Kevin,
After a shaky start, I am so pleased for you that it has all gone to plan now. You, your family and friends must be overjoyed, and quite rightly so. An inspirational story.
This comes as a good news story to me as I may face a similar thing in the future. Recently diagnosed with IPF, so I am (hopefully) a long way off yet.
Enjoy your new lease of life!
Kind regards
Jeff (in the UK)
Kevin Olson
Good Day, Jeff. Yes, my family and friends are ecstatic over my recovery. It was six years after first being diagnosed with IPF when I had the transplant. I hope your time between diagnosis and transplant is longer than mine. Thank you for reading my column. Kevin
BERT Maidment
Go Kevin Go —- Proud of you man!
Kevin Olson
Thank you, Bert. Go, Team Bert!
Allan Byro
So happy to hear of your progress. Where did u had your transplant? I hope I can do the same. I am 73 years old, and want
a transplant if possible
Kevin Olson
Allan, Thank you for reading my article. I had my transplant at Barnes Jewish Hospital in St. Louis, MO (USA). I have two good friends in their 70s who had their transplant after me. They are doing well. Rooting for you.
Kevin
David Maynard
Thanks for sharing...and `May the Force be with you'!
Kevin Olson
Thanks for reading my story. And May the Force be with you!
Debbie
Kevin,
Thank you so much for sharing your story. It is an inspiration to me. I have been trying to read as many stories as possible. I have my first appointment with a lung transplant team on September 1st and no idea what to expect or anything. I have a positive attitude about everything and definitely try not to worry or over think anything until I know facts. I am really happy you are doing well and hope you continue to enjoy life to the fullest.
Blessings,
Debbie
Kevin Olson
Thank You, Debbie, for reading my column and the kind words. I am glad to see that you have an appointment. You will do fine with your positive attitude. Best of luck. Kevin
Lydia Rogers
Very inspiring Kevin. I had my transplant August 1, 2021 and am taking baby steps toward full recovery. I look forward to traveling again and really showing off my stamina.
Kevin Olson
Congratulations on your transplant. My surgeon said it would take a year to recover with many ups and downs fully. Always stay positive. You will get there.
Janis Consolver
Thank you Kevin for sharing your incredible story! Husband is on day 2 and I know we have some tough days ahead. We are so blessed with his initial progresses so far. This is a marathon and not a sprint. Just one day at a time. We are down one, 364 days to go
Kevin Olson
Janis. You are welcome. Prayers for your husband's successful recovery.