I Have COVID-19. Here’s What Happened
Written by |

I am taking a deep breath as I announce to my beloved online community the following: I have COVID-19. I also have idiopathic pulmonary fibrosis (IPF). Until now, I thought this combination would be fatal, but I am here to tell you that this isn’t necessarily true.
I’m a fairly private person, contrary to popular belief considering I’m a columnist writing about life with a chronic lung disease, so initially I didn’t want to share this news publicly. However, I feel obligated to share my COVID-19 experience with the pulmonary fibrosis community.
One word I might use to describe the experience is “chaos.”
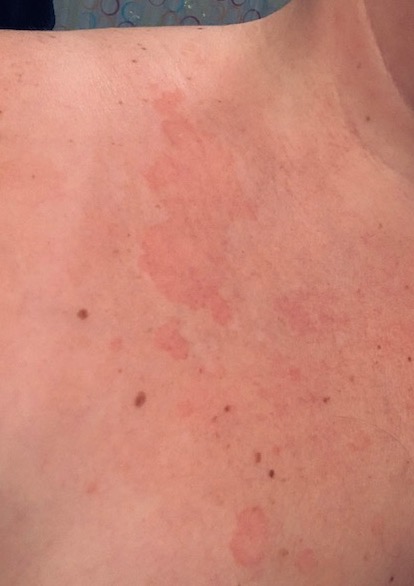
After waking up with a 102-degree fever, a headache, and chills so bad I wanted to crawl out of my skin, I was initially swabbed for COVID-19 as a high-risk patient over three weeks ago. My doctor told me she had decided to send me to the emergency room after noticing a rash that developed on my chest two days after the initial symptoms appeared. The rash prompted the ER doctor to swab me.
In addition to a chest X-ray, I had bloodwork done that showed significantly elevated C-reactive protein, a marker of inflammation.
The intense symptoms of fever, headache, and chills began to subside within days of first appearing. I also experienced muscle fatigue and general malaise. I anxiously awaited my swab results to be uploaded online, but my doctor called first, saying my test was negative.
We both were surprised, as the symptoms I’d been experiencing felt unlike any virus I’d ever had. My doctor noted that my bloodwork wasn’t indicative of a bacterial infection that might have explained the high fever.
We decided to wait, and she called every day to check in. She trusted me to self-monitor my symptoms, given my knowledge of IPF and how it affects my body .
While my first COVID-19 swab was two days after the onset of symptoms, my second one happened 11 days later. By then, the intense symptoms of fever, persistent headache, and chills mostly had subsided, but I was now experiencing respiratory symptoms. As an IPF patient, this made me anxious and scared.
When my doctor called again, she learned that my shortness of breath had worsened and that I’d developed a dry cough, especially during inhalation. I told her I also had pressure in my chest that felt like someone was cupping their hands around my rib cage and squeezing. She sent me to an assessment center to be swabbed again. The second swab came back positive for COVID-19.
As the respiratory component of the virus worked its way through my system, I was hospitalized a couple times because I needed higher amounts of oxygen than my portable oxygen concentrator and tanks could provide. I reduced my oxygen needs, albeit slowly, and returned home within a couple days of going to the hospital each time.
More than four weeks have passed since the start of my symptoms, and I believe I have beaten COVID-19. However, before I am considered officially recovered, I need to be swabbed two more times at least 24 hours apart, and each needs to be negative.
I will be swabbed again in a couple of days, so we’ll see what that reveals.
While the physical symptoms of COVID-19 have nearly subsided, I have a lot of work to do with the emotional side of this virus. It is scary knowing I have an illness that has killed so many people around the world, and that is constantly making headlines in the news.
The hardest part for me was telling those I love most that my second swab came back positive for the virus. Some cried because of fear and anxiety, and I couldn’t do anything to comfort them other than reassure them that physically, I was OK.
When I hear the word “COVID,” I now feel triggered and tearful.
The emotional aspect of having this virus also will subside with time, but it was one of the reasons I didn’t want to share with the PF community that I was COVID-19 positive. However, my commitment to this community is to always be transparent and honest to those living with IPF. I want to share with you that given my experience, contracting COVID-19 as a patient with IPF is not always fatal and can be managed.
Stay safe out there, friends.
***
Note: Pulmonary Fibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Fibrosis News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary fibrosis.




Michele
Thank you so much for sharing your experience Charlene! I am so glad you’re doing better. I have been lurking on the forums since I was diagnosed last July but never posted. You have faced what we are all fearing and it would appear you have won! This will provide so much hope to all of us. I had a telephone appointment with my Dr. I in early April and asked her if there would be a possibility I could survive Covid-19 if I got it and her response was “not a chance”. So well done and keep up the good work!
Charlene Marshall
Hi Michele,
Thank you so much for reading my columns and reaching out via the comments. I'm so glad you're part of our forums community, even just as a member who reads; I hope it has been helpful for you. I truly can say, I believe I have beaten COVID-19 as a patient with compromised lungs, I am just waiting for the swab result(s) to confirm but based on my symptoms, I am almost 100% again. I was uncomfortable with sharing this news at first, because the last thing I wanted to do was worry others, but then I felt like I had an obligation to hopefully provide some ease to other patients. I am still, of course, advocating that everyone take their utmost precaution to avoid getting it but I also didn't have as difficult of time with it as I anticipated. I'm disappointed to hear your doctor said that, the truth is, no one knows for certain. Stay healthy and thanks again for writing :)
Ron Reid
Charlene: Thank you for sharing this; and so sorry that you have had to go through the Covid experience. As someone over 70 with IPF, I have also assumed that catching Covid would be a death sentence. So it is somewhat reassuring to hear that you have survived. We greatly appreciate all your talent in pulling together PFNews, and especially your columns. Godspeed for a full recovery from Covid; in the meantime, I and many others will continue to self-isolate.
Charlene Marshall
Hi Ron,
Thank you so much for reading my column and reaching out via the comments. I had those same thoughts; that catching COVID while living with IPF would almost certainly be fatal, even despite the age difference. As a result, I was very scared when my swab came back positive. I am glad it is reassuring to read my story! I am still, of course, encouraging everyone to take all proper precautions to avoid getting the virus, but I also hope it provides some comfort too. Continue to self-isolate and stay safe!
Charlene.
Shirley Leeper
What wonderful news that you have recovered from covid 19. Guess I just assumed at age 92 I would be a goner if I got it. I know you are so much younger than I but IPF we all have to extremely careful. Hang in there Charlene I read your column and pray for you everyday.
Charlene Marshall
Hi Shirley,
Thank you so much for reading my column and connecting via the comments. It is nice to hear from you, and I appreciate your kind words. While not officially recovered yet, as I have to wait for two consecutive swabs that are negative (I have one so far!).. I am indeed feeling almost 100% better. While unpleasant for a few days, I truly believe I ended up with a mild case of COVID which I am thankful for. What I neglected to mention in the article is, as you say, remaining extremely careful and vigilant is important for all of us. Take good care, and thank you again for your kind words and prayers! :) Charlene.
Cassie
My 77 year old husband with IPF got Covid at the end of December. He got monoclonal antibodies the first week in January. He was having pain in his chest when he took a deep breath, & so I asked his doctor about having a CT scan, which was done. It showed his lungs were filled with inflammation. They did a bronchoscopy & took biopsies, & he has Organizing Pneumonia, which is very rare. He's taking a large dose of Prednisone for 28 days, along with an antibiotic 3 days/week. He's feeling fairly good, & we see his lung disease doctor in a week, when he'll also have a pulmonary function test. Anxious to get those results & see what the next steps will be. But so far, so good- looks like someone with IPF can survive Covid, & hopefully Organizing Pneumonia, too.
Charlene Marshall
Hi Cassie,
Thanks so much for reading my columns and reaching out via the comments. Sorry to hear your husband ended up with COVID and subsequent lung inflammation. This virus is so unfair! I'll keep you in my prayers for seeing the lung disease doctor and hope the function tests are okay. Thanks for sharing his story, and I'm glad to hear, despite everything, he is feeling quite good.
Take care,
Charlene.
Piet Potgieter
Holding thumbs for you, Charlene!
Charlene Marshall
Thank you so much my friend! Stay safe Piet, and thanks for being such a wonderful member of our forums and PF community. Hugs, Char.
Terril McBride
I am so glad you beat this. It's encouraging to know that a person with IPF had covid19, and got better. It makes me a little less terrified.
Charlene Marshall
Hi Terril,
Thanks so much for reading my columns and reaching out via the comments. I so appreciate your kind words! It was hard to "go public" with this information, but I was hopeful it would ease some anxiety for the IPF/PF community. Of course, it is imperative we do our best to avoid it, but I wanted to share a 'good news' story too. Thanks for writing! Charlene.
Barbara Mathis
Tried to leave a five star rating, as I clicked one, my intention was to mark all five. After clicking one star, it already rated the comment. Charlene is wonderful in her work to communicate with other IPF patients.
Charlene Marshall
Hi Barbara,
No problem at all, thank you so much for reading my column and for the 5-star rating! I appreciate your kind words, and thank you for being such a wonderful part of our community. I truly believe we're better together!
Bill K.
Charlene - thanks so much for sharing your experience with us The thought of getting COVID-19 at age 73 with IPF terrifies me, but I haven't let that fear take over my life. It does compel me to be very careful about where I go, what I do, and who I deal with. So far my town and county have had very few cases of COVID and we do hope to keep it that way. Haven't been to church for two months but we have been conducting weekly Sunday services on YouTube which has helped, and we have a virtual coffee hour after the service where we can see and talk to our good friends - about as close to normal as we can get. I am glad that you are recovering, it gives us all hope that there is a future after COVID-19. Hoping for your full recovery from the virus.
Charlene Marshall
Hi Bill,
Thank you so much for reading my columns and reaching out via the comments. Like you, I was terrified of contracting the virus as a patient living with IPF and ironically enough, we traced it back to getting it from a hospital. I'm glad you haven't let the fear take over your life, that is important and I'm so glad you continue to take precautions when it comes to all interactions and errands. Despite my surviving it, I should have also included in the article that I am of course still encouraging folks to take all proper precautions to avoid getting the virus. So glad you have virtual options to continue being connected to your community, this is so important. Hang in there, and thanks again for writing. Stay safe! Charlene.
Nicole Medina
Hi Bill,
I contracted COVID 19. I live with my father, 78 and he has IPF. He's starting to get sick and will be tested tomorrow. What was your protocol and any tips would be a godsend. I'm so nervous I'm going to be the culprit for my father's death.
Thank you,
Nicole
Pam Gilbertson
I'm so sorry to hear you had to go thru this. Thank you for sharing with us, as of course it gives a positive to those of us afraid of contracting the virus. I have PF (hypersensitivity pneumonitis) and have and continue to shelter at home to avoid getting it as much as possible but as my family has to go out on occasion it is still possible I could be exposed.
Good luck as you continue to recover. I wish you all the BEST !
Charlene Marshall
Hi Pam,
Thank you so much for reading my column and for your kind words! My hope was that it would give some encouragement/hope/support to those fearful of catching the virus. It is, of course, very important that we continue to take all precautions to avoid getting the virus but I also wanted to share that I managed with it quite well, as a patient with a lung disease. The possible exposure is scary, but I hope you continue to stay well. Thank you so much for your well wishes :)
Cynthia R Chase
Thank you for sharing. I am 79, diagnosed this past December. Have yet to come to terms with this, and very resentful of having lost the good health I enjoyed most of my life. Another loss was the ability to sing.
Charlene Marshall
Hi Cynthia,
Thanks so much for reading my column and reaching out via the comments. The resentment for what this disease takes from us is very normal, albeit very hard to accept. It is truly unfair, and I'm so sorry you've lost the ability to sing. Be gentle with yourself in these months following your diagnosis; I remember them well and they sure are so hard to deal with. Take good care, and reach out anytime, Charlene.
Suzanne
Charlene, thank you so much for sharing your story. I'm sure it was unbelievably scary while you were going through it and I'm just so glad you are on the mend and that you shared your experience. I believe that as time goes by, the emotional aspects of that time will fade although never truly go away.
As another IPFer, I live in dread of catching it and haven't left my house since March 9 to try to minimize the risk of catching it. I am quite a bit older than you are but try to eat well and exercise to the extent I can however I know that my chances of being able to beat COVID-19 are slim.
Thank you and take care as you recover.
Charlene Marshall
Hello my friend,
Thank you so much for reading my columns, and as always, it is wonderful to hear from you! You're right - it was very scary when my swab came back positive, but my Doctor was so good. I'll never forget the look she gave me when she locked eyes with me (sounds romantic, ha!) and reassured me this did not mean I was going to succumb to the virus, as I had previously assumed. She was right! I have some work to do about he emotional aspects of the virus for sure, but with time, I'll get there. Sharing my story via this column, though not something I wanted to do at first, has been very therapeutic and comforting to know it has helped others.
I am glad you continue to take all precautions to avoid getting it, this remains top priority for those of us with IPF. Stay safe, and thanks again for writing :)
Charlene.
Robert Bell
Charlene, thanks for sharing and being so open. I'm going to ask my doctor for the antibody test next month. I was sick for 5 wks earlier this year. All the symptoms were there. My first test showed I had flu type A, immediately following that I went back to see if I still had it and I didn't. They said it wad a bacterial infection but they didn't do blood work. Then thre next week I had an ear infection. I had been dizzy for 5 wks and then it began to hurt. All of my symptoms could have been the seperate diagnosis but when I look at all the symptoms it could have been Covid. I was in bed a lot with chills, dizzy, lousy my appetite, nothing tasted right, I broke out in a rash, I had diarrhea and even passed blood. I wasn't coughing a lot but that was because I tried not to move fast. It was hard to breathe. Of course, I'm on oxygen at 3 liters.
It may have just been several different things but it was at the very beginning of Covid, and was just after I'd been on a domestic flight. Anyway, your article triggered that. I'm doing great now and have even started walking everyday. If I'm tested I'll let you know.
Charlene Marshall
Hi Robert,
Thanks so much for reading my columns and reaching out via the comments. Do let me know what your doctor thinks about the antibodies test, it would be really interesting to hear multiple medical perspectives on this, as I haven't heard yet that this is available. Unfortunately, the loss of taste and rash are what-my-doctor called "rapidly emerging symptoms of COVID". So sorry you endured this Robert, it is truly awful. I'm glad you've recovered, but do let me know what they say about the COVID antibodies test... kudos to you for walking every day, I know that isn't easy when dependent on 02. Sending you much love!
Charlene.
Holly W Patient
We love you, Charlene.
Charlene Marshall
You're such a beautiful friend, Holly (& Christie, too!). So much love back to you both. Thank you for your kind words. xoxo.
Roger Coles
Hi Charlene, thank you very much for your story and I think your story and the emotional roller- coaster that you have gone through is something that's on the mind of many IPF sufferers. While I have been very lucky with my IPF over the past 3 years, I am constantly watching the developments of COVID in Australia and around the world. I had a COVID swab in hospital last week (nothing to do with IPF) which showed I was negative, but see by your tale that "one swallow doesn't necessarily makes a summer". Since coming home from hospital have been tired, coughing more than I ever did in the 3 years previously. Plus, I seem to have a demand for air which I prior going to hospital. While in hospital the doctors said I appeared to have a virus but couldn't identify the exact nature of this, and had my annual fluvac (vaccination) some 7 weeks previously. Additionally, I am finding my fingers seem to be cold all the time - again something I never had before. So I think I will watch the next week and see what develops. Charlene, once again many thanks for you story which effects all of us. While I am 74 I would like to use up all the frequent flyer points I have amassed once this international health scare is over.. Keep fighting, regards PS If you finally get to come Down Under (Australia) and we have been very lucky with the numbers of deaths we have had from CORONA 19, please let me know, as I would think one of the biggest hospitals we have in Melbourne could organize a catch up with other IPF members in the city.That is if you would like to meet other members and get to chew over the steak on our common and different conditions. Please let me know, as we are a reasonably friendly lot.
Rating 5 STARS
Charlene Marshall
Hi Roger,
Thank you so much for reading my column and reaching out via the comments. As always, it is wonderful to hear from you my friend. I have been thinking of many of my friends and "family" down under often, especially with how difficult the start of the year was for many of you, with the fires! I'm really glad your first swab was negative Roger. While the "error rate" of a false negative is only between 5-10%, it does unfortunately happen and did to me. There is so much they are still learning about this virus, and I wanted to write about my experience to educate others. The cold fingers and hands is something I had too! I spoke with my GP often about this actually. How irritating for you. Have you improved anymore since writing me this note? It will be interesting once an antibody test is developed to see if you had the virus or not.
I had hoped to come to your beautiful part of the world in 2020 actually, Roger! Sadly, it looks like it might have to be 2021 at this rate but I do plan on coming back. Is the hospital you're referring to The Alfred? I have an amazing friend there, who had a transplant and is ambassador for the hospital's transplant program and Lung Foundation Australia. I want to visit him and his family again! I would love to organize a gathering in Melbourne, how amazing would that be? Let's keep a dialogue open about this!!! Take good care, and I hope you continue to feel better. Write anytime, Roger.
Hugs to you, Charlene.
Maureen Terhune
Hi Charlene,
First of all I want to thank you for sharing your COVID-19 diagnosis with those of us who follow your postings. It can't have been easy. But you can't imagine what a difference it makes to know that this disease is survivable even when someone has PF. I had presumed that there wasn't much chance of doing that. You have given so many of us hope in these bleak times.
Our province has had few cases of the virus and so far there have been no deaths. We are in a Yellow Phase with some relaxed rules, but my husband and I continue to act as if we were still in the Red Phase. It's safer! Yesterday it was Day 70 of our personal lockdown. Our hair is getting longer - but of course this is trivial compared to what is going on.
I did wonder where you could have contracted the virus as I am sure you would have been super-cautious. So having learned it was at the hospital, I think I was right to be scared about going to our hospital for routine things. Luckily most of them were cancelled. But when I had to see my family doctor I realised I was really nervous about going to an inside place, and think it was because I hadn't been inside anywhere except my own home for almost ten weeks. Maybe others have been experiencing anxiety when going to appointments etc.?
All the very best to all who follow this site. May you all stay well. And thanks to Charlene for her encouragement and this latest sign of hope.
Maureen
Charlene Marshall
Hi Maureen,
Thank you so much for reading my columns and sharing such kind words via the comments. They truly mean a lot to me, especially after a bit of a difficult day... thank you! I had hoped my sharing, as difficult as it was, would provide some hope and comfort to those very anxious about the virus. One thing I neglected to mention was of course, the importance of still doing everything we can and taking all proper precautions to avoid getting the virus if we can. Ironically enough, we contact traced my exposure back to a hospital!
It is so hard to see some parts of Canada having irresponsible citizens that are extending this lockdown even longer. I know it is important not to open up until it is truly safe, so I agree with you, the personal lockdown is important. I am alongside you and your husband, at day 80 I think.
It does sound like many are sharing that same anxiety with you my friend, about going out in public after being in lockdown for so long. Did you have your appointment yet? I hope it went well.
Take good care and feel free to write any time! I truly believe we're better together :)
Charlene.
Wendy Dirks
I am so terribly sorry you have had to go through this, especially after being so ill last year. What a nightmare. But most of all, I am so glad you survived. I'm sending you a virtual hug. I can't imagine what we do without you. Much love, Wendy
Charlene Marshall
Hi Wendy,
Thank you so much for writing my friend, it is wonderful to hear from you, as always! After a difficult afternoon, your kind words really lifted my spirits, thank you. It was pretty scary to be diagnosed COVID+, especially after being so careful and only being exposed while having to go for a routine appointment. It was scary mentally, but also disappointed emotionally. Still working through that part! Thank you again for writing - sending big virtual hugs back to you. Much love, and thanks again, Charlene.
Karen
As I read your column I was thanking God for protecting you and bringing you through this. You have become such a positive and honest warrior for all of us. You bring hope to all us. Thank you fir being so open with us. It’s been a real struggle. I’m in the middle of an exacerbation and just had to up my Prednisone to 60 mg a day to be able to function at all. You gave me the much needed push to get over this and move on. Praying for you daily Charlene. ?
Charlene Marshall
Hi Karen,
Thank you so much for your kind words and comments on my COVID-19 experience. It's kind of like God/karma/fate (whichever your preferred belief is) brought me to your comment today, as I've just finished a really tough day and your words lifted my spirits greatly. Thank you! I'm so sorry to hear of your exacerbation, those are so tough and Prednisone is such an unpleasant drug. Be gentle with yourself both physically and emotionally as recovering from any type of acute setback is hard work. I just finished a column about this exact topic, which will be published on Thursday. Thank you again for your kind words Karen, please know how much they helped me today. I appreciate you and sending love and prayers back to you. Please write any time!
Hugs,
Charlene.
Karen Gonsler
I’m feeling much better and appreciated your kindness. It’s a love hate relationship with prednisone. I tried so hard to lower it but I’m realizing it’s not worth it. I need to be able to at least function somewhat. I’m down to 50 for a week then 40 etc. Trying hard to stay positive and it’s working. Thank you for your kind words and I’m glad I could help you even if just s little yo lift you up.
Continuing prayer for you. ??
Charlene Marshall
Hi Karen,
Thank you so much for circling back and letting me know how you're doing - I've been thinking of you! I couldn't agree more, that love-hate relationship with Prednisone. The taper is always tough for me to do too, especially after an acute event like it sounds you had. Hang in there, and so glad you're on the mend now! Wishing you nothing but the best, keep in touch!
Charlene :)
Betty Supinski
Thank you so much for sharing your experiences with us. You are way too young to have a lung problem. I am a woman dealing with IPF but I am in my 80's. Hopefully you will get stronger and stronger and fight this lung disease with ever part of your body. GET WELL AND GOD BLESS YOU FOR SHARING.
Charlene Marshall
Hi Betty,
Thanks so much for reading my columns and getting in touch via the comments. I also appreciate your kind words - unfortunately this cruel disease does not discriminate when it comes to age, does it? I am getting stronger each day, though still quite tired and overwhelmed some days. Comments that my column has helped others, helps me to keep going so thank you for writing Betty. Take care, and wishing you all the best!
Charlene.
Jerry Genesio
Thank you for sharing this with us Charlene. It helps a lot just knowing survival for an IPF patient is a possibility. I live in Maine where the risk is very low compared to most states, nevertheless, there is risk everywhere. I'm 81 so I'm literally taking every possible precaution, still there is risk everywhere. Again, thanks for sharing! Your survival is some of the best COVID-related news I've heard this year.
Charlene Marshall
Hello my friend,
Thanks so much for reading my column and reaching out with your kind words! What I realized (in hindsight of course) is that I forgot to mention in the article, that it remains of paramount importance to take precautions and eliminate the risk of contracting COVID-19 as much as we can as IPF patients, as you mention you are. However, I did also want to share that it is possible to survive it if we do get it, despite our best efforts. Thanks for your kind words - keep your fingers crossed that my PFTs in a few weeks don't show any permanent or significant damage done by the virus. I do feel more SOB, but who knows what that could mean. As we know, that could be attributed to many different things! Thanks again for writing, and "see you" on the forums :)
Charlene.
Sybil Sutton
Hi Charlene,
Thank you for sharing with us. I am thankful that you have apparently been able to beat C19. Have you any idea as to how you may have contracted it?
I trust that all future tests will be negative as well.
Charlene Marshall
Hi Sybil,
Thank you so much for reading my columns and for reaching out with such kind words! It was a tough decision about whether or not to share I'd been diagnosed with COVID-19, but I'm glad I did now. I have beaten it, but I am what they call a "long hauler", meaning I'm still having some issues despite testing negative for the virus now. Some GI and cardiac manifestations, which is tough to accept. We contact traced it back to my hospital visit at the end of April unfortunately, as I'd not been anywhere else. Thanks again for your kind words Sybil, I hope you're keeping well.
Sincerely,
Char.
Sybil Sutton
So thankful you seem to have beat C-19. ♥️
Stefanie Ellenberg
Thank you so much for writing your story. My mom has PF and had a positive Covid test just yesterday. I have been trying to find information on the two together ever since. Your story was the first and only one I came across that had useful information and addressed the topic directly. Not only that, but you have just given me so much hope that all will be fine. Thank you so much for sharing.
Charlene Marshall
Hi Stefanie,
Thank you so much for reading my column and reaching out via the comments. I'm sorry to hear your Mom, who has PF, has been diagnosed with Covid-19. I think one of the scariest things for me was the mental anguish and anxiety it caused when my test was positive as well. I have two friends who are both post double-lung transplant who have also had Covid and done well. I hope your Mom does well also, and remains positive: while the physical symptoms were unpleasant, keeping my "head on straight" was important too. Please feel free to reach out if you have any other questions.
Sincerely,
Charlene.
Nicole Medina
Hello Charlene,
First I'm glad you're on the mend and recovered.
I contracted COVID 19. I live with my father, 78 and he has IPF. He's starting to get sick and will be tested tomorrow. What was your protocol and any tips would be a godsend. I'm so nervous I'm going to be the culprit for my father's death. And my siblings are giving me the 4th degree and saying this is all my fault. I'm so scared for my father.
Thank you,
Nicole
Charlene Marshall
Hi Nicole,
Thanks so much for writing and reaching out via the comments. So sorry to hear you contracted COVID-19. How are you doing, and has your father tested positive/how is he doing? The first recommendation I can make is to not let the mental anguish or anxiety consume you. This is so tough, and I stand firm that one of the hardest parts of me getting COVID was the mental anguish and worry that came with it. If it helps, I know several patients with IPF (some post-lung transplant too) that have done well, despite COVID. Of course everyone's situation is different and I hope your Dad's course with it isn't too difficult. Please let me know how he is doing when you can, and I hope you're on the mend too.
Charlene.
William
I am a 75 year old man with Pulmonary Fibrosis caused by pneumonitis. I was taken to emergency 28 days ago as I had developed severe shortness of breath over the past few days. Three weeks prior to that I severe diarrhea and chills . I was diagnosed in emergency as having COVID 19. I have remained in hospital since then(28 days so far) . I have survived the COVID but it has damaged my lungs to the extent that Initial O2 ventilation was at 80% 02 concentration. I am currently at 10 litres O2 at rest and increase to 25 litres when I need to get out of bed to exercise ,150 steps yesterday. My prognosis is good as I continue to demand less supplemental o2 over time . I expect to return home in about two weeks. I will say that with PF and an immune system suppressed by mychopenolate I knew I could not avoid COVID 19 so I a year and a half ago I began a Weight loss and exercise program to increase my survival odds. A time of COVID I had lost 42 pounds and was walking an hour daily and doing 30 minutes a day anaerobic with dumbbells. I believe it paid off. Thank you for your News Charlene.
Charlene Marshall
Hi William,
Thank you for reading my column and sharing your experience with COVID-19. I'm so sorry that happened to you, but your commitment to exercise likely paid off when you did catch it. I agree, I was resigned to the fact that I likely couldn't avoid it either. I hope you continue to improve and trend in the right direction! Thanks for sharing your story and wishing you all the best in your continued recovery.
Charlene.